What Causes an Enlarged Prostate (BPH)? Hormones, Age & Risk Factors
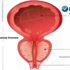
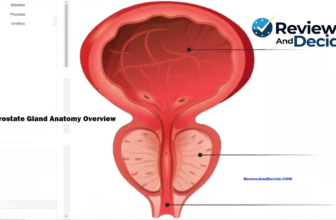
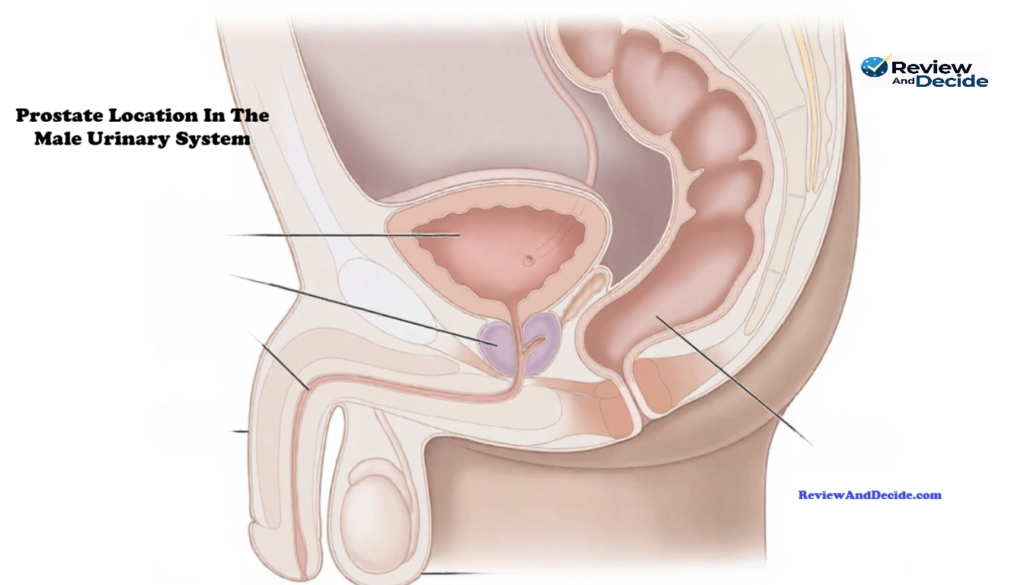
What causes an enlarged prostate (BPH)? Learn how aging, DHT, hormonal balance, and lifestyle factors influence prostate growth after 40 in this research-informed educational guide. The prostate is a small gland located just below the bladder and in front of the rectum. It surrounds the urethra — the tube responsible for carrying urine from the bladder out of the body. In younger men, the prostate is typically about the size of a walnut and weighs approximately 20–25 grams. Its primary biological role is to produce seminal fluid, which nourishes and transports sperm during ejaculation. While this reproductive function is well understood, the prostate’s location within the urinary system explains why enlargement can affect urination. Because the urethra passes directly through the prostate gland, any increase in prostate size may narrow the urinary channel. Over time, this narrowing can lead to urinary flow changes, particularly in aging men.
(For a more detailed overview of prostate anatomy and function, readers can refer to our main educational guide on the prostate gland.)
Primary Causes of Prostate Enlargement
Benign prostatic hyperplasia does not result from a single cause. Instead, it appears to be influenced by a combination of hormonal, cellular, and age-related factors.
Hormonal Changes With Age
As men age, testosterone levels gradually decline. However, this does not mean prostate growth stops. In fact, research suggests that hormonal balance — rather than absolute hormone levels — plays a key role.
Two hormones are particularly important:
- Testosterone
• Dihydrotestosterone (DHT)
Testosterone can be converted into DHT by an enzyme called 5-alpha reductase. DHT is a more potent androgen (male hormone) that binds strongly to receptors in prostate tissue.
Even as circulating testosterone declines with age, DHT levels within the prostate may remain active. Some researchers suggest that prolonged exposure to DHT may stimulate continued prostate cell growth.
(A deeper exploration of this mechanism will be covered in our upcoming article on how DHT affects the prostate.)
Dihydrotestosterone (DHT) Accumulation
DHT is essential for prostate development during puberty. However, in adulthood, persistent DHT activity may contribute to gradual enlargement.
Studies have shown that:
- Men with BPH often have measurable DHT levels within prostate tissue
• Blocking DHT production can reduce prostate volume in some cases
• Genetic sensitivity to androgens may vary between individuals
This suggests that BPH may partly result from how prostate cells respond to hormonal signals over time.
Importantly, this process is slow and typically develops over decades.
Estrogen Balance in Aging Men
Another factor sometimes discussed in research is the changing ratio of testosterone to estrogen as men age.
Although estrogen is commonly associated with female physiology, men also produce small amounts. With aging, relative estrogen levels may increase as testosterone declines.
Some researchers propose that shifts in hormonal balance could influence prostate cell activity, though this area remains under investigation.
Current evidence suggests that hormonal interplay — not a single hormone — influences prostate enlargement.
Risk Factors Associated With BPH
While aging is the strongest risk factor, several additional factors have been associated with increased likelihood of BPH.
Age
Age is the most significant predictor. Prostate growth patterns typically follow this pattern:
- Minimal enlargement before 40
• Gradual increase after 50
• High prevalence after 60
By age 70, a large percentage of men show some degree of prostate enlargement.
Family History
Genetics may influence susceptibility. Men with a family history of prostate enlargement may develop symptoms earlier.
Obesity and Metabolic Factors
Research has examined possible links between:
- Obesity
• Insulin resistance
• Type 2 diabetes
• Metabolic syndrome
Some studies suggest that metabolic health may influence inflammatory pathways and hormonal regulation, which could indirectly affect prostate tissue.
However, these relationships are complex and still being studied.
Sedentary Lifestyle
Lower physical activity levels have been associated in some studies with increased urinary symptoms. Physical movement supports cardiovascular and metabolic health, which may influence overall hormone balance.
While lifestyle alone does not “cause” BPH, it may play a supportive role in long-term health patterns.
Common Symptoms of an Enlarged Prostate
BPH symptoms generally develop gradually. They are primarily related to urinary function due to pressure on the urethra.
Common symptoms include:
- Frequent urination
• Urgency
• Weak urine stream
• Difficulty starting urination
• Dribbling at the end of urination
• Feeling of incomplete bladder emptying
• Nighttime urination (nocturia)
Symptoms can vary in severity. Some men with significant enlargement experience mild symptoms, while others with smaller enlargement may notice more disruption.
This variability is one reason why individual medical evaluation is important.
Is BPH Preventable?
Aging is a natural biological process, and prostate enlargement is common in older men. There is currently no guaranteed method to completely prevent BPH.
However, maintaining overall metabolic and cardiovascular health may support balanced hormonal function.
Research continues to explore how:
- Weight management
• Regular physical activity
• Balanced nutrition
• Sleep quality
may influence long-term prostate health.
It is important to understand that lifestyle adjustments may support overall wellness but do not replace medical guidance.
When Should Someone Speak With a Healthcare Professional?
While mild urinary changes are common with age, certain symptoms warrant medical evaluation.
Individuals should consider speaking with a healthcare professional if they experience:
- Difficulty urinating
• Inability to urinate
• Blood in the urine
• Pain during urination
• Recurrent urinary infections
Early evaluation helps rule out other conditions, including prostate cancer or bladder issues.
Educational content such as this article is not a substitute for individualized medical advice.
How BPH Is Diagnosed
Healthcare providers may use several tools to evaluate prostate enlargement.
Medical History and Symptom Assessment
A symptom questionnaire may be used to assess severity.
Digital Rectal Examination (DRE)
A physical exam allows assessment of prostate size and texture.
Prostate-Specific Antigen (PSA) Test
PSA is a protein produced by prostate cells. Elevated levels can occur in BPH, inflammation, or prostate cancer. PSA alone does not diagnose BPH but may be part of a broader assessment.
Imaging
In some cases, ultrasound imaging may be used to measure prostate volume.
Urine Flow Studies
These tests measure how effectively urine flows from the bladder.
Current Medical Management Approaches (Educational Overview)
Treatment decisions depend on symptom severity.
Watchful Waiting
For mild symptoms, monitoring may be sufficient.
Medications
Some medications work by relaxing prostate muscles, while others reduce DHT production.
Surgical Procedures
In severe cases, minimally invasive procedures may remove excess tissue.
This article does not recommend specific treatments. Decisions should be made in consultation with qualified medical professionals.
Research on Natural Compounds for Prostate Support
Several plant-based compounds have been studied for their potential role in prostate support.
Saw Palmetto
Some clinical trials have examined its role in urinary symptom relief, though results have been mixed.
Beta-Sitosterol
This plant compound has been studied for urinary flow improvement in some small studies.
Zinc
Zinc plays a role in cellular health and immune function. Its direct effect on BPH remains under investigation.
Scientific findings in this area are still evolving, and individual responses may vary.
Key Takeaways
- BPH is a common age-related condition
• Hormonal balance, particularly DHT, may influence growth
• Aging is the strongest risk factor
• Symptoms primarily affect urination
• Diagnosis involves medical evaluation
• Management depends on severity
• Lifestyle may influence overall prostate health
Frequently Asked Questions (FAQ)
What is the main cause of BPH?
Aging and hormonal changes, particularly involving DHT, are considered primary contributors.
Is BPH the same as prostate cancer?
No. BPH is non-cancerous and does not directly cause cancer.
At what age does prostate enlargement begin?
It commonly begins after age 40 and becomes more prevalent after 50.
Does testosterone cause prostate enlargement?
Testosterone itself is not considered the sole cause. Its conversion to DHT plays a role in prostate tissue activity.
Can lifestyle changes reverse BPH?
Lifestyle factors may support overall health but do not guarantee reversal of prostate enlargement.
Conclusion
Benign prostatic hyperplasia (BPH) is a common age-related change that affects many men after the age of 40. While the condition is not cancerous, its gradual development reflects complex interactions between hormonal balance, cellular growth patterns, and the natural aging process.
Current research suggests that dihydrotestosterone (DHT), shifts in testosterone levels, genetic predisposition, and broader metabolic factors may all contribute to prostate enlargement over time. However, BPH does not result from a single cause, and its progression can vary significantly between individuals.
Understanding what causes an enlarged prostate helps place symptoms in proper context. Urinary changes may occur gradually, and their severity does not always correspond directly to prostate size. This variability highlights the importance of individualized medical evaluation when concerns arise.
While lifestyle factors such as physical activity, balanced nutrition, and overall metabolic health may support general well-being, they are not guaranteed methods of prevention. Decisions regarding diagnosis, monitoring, or treatment should always be guided by qualified healthcare professionals.
By approaching prostate health from a research-informed and balanced perspective, men can engage in informed discussions with healthcare providers and better understand the biological processes that occur with aging. Education promotes clarity — not alarm — and supports responsible, evidence-based health awareness.
explore more evidence-based prostate health articles
Medical & Educational Disclaimer
This article is provided for educational and informational purposes only. It is based on publicly available research and guidance from recognized health authorities such as the National Institutes of Health (NIH), National Institute on Aging (NIA), Harvard Health Publishing, and the Centers for Disease Control and Prevention (CDC).
Benign prostatic hyperplasia (BPH) is a medical condition that should be evaluated by a qualified healthcare professional. This content does not provide medical diagnosis, treatment recommendations, or individualized health advice.
Hormonal balance, prostate growth, and urinary symptoms can vary significantly between individuals. Anyone experiencing persistent or severe urinary symptoms should consult a licensed healthcare provider for appropriate evaluation and guidance.
Individual results and health outcomes may vary.
 High-Authority References
High-Authority References
National Institute on Aging (NIA)
National Institutes of Health (NIH) – Benign Prostatic Hyperplasia
Harvard Health Publishing – Enlarged Prostate Overview
Cleveland Clinic – Benign Prostatic Hyperplasia (BPH)
Centers for Disease Control and Prevention (CDC) – Prostate Health Information