What Is the Prostate? Function, Anatomy & Age-Related Changes Explained
What is the prostate and what does it do? Learn about prostate function, anatomy, and how prostate health changes with age in this research-informed guide. The prostate is a small gland that forms part of the male reproductive system, yet its biological significance extends beyond what many people realize. Although it is often discussed in connection with aging, urinary symptoms, or men’s health screenings, the prostate is fundamentally a normal anatomical structure that plays a defined physiological role throughout adult life.
According to the National Institutes of Health (NIH), the prostate contributes fluid to semen and functions in coordination with other components of the male reproductive system. This fluid supports sperm mobility and viability. While the gland itself is modest in size — approximately the size of a walnut in younger adult men — its location and hormonal responsiveness make it biologically important.
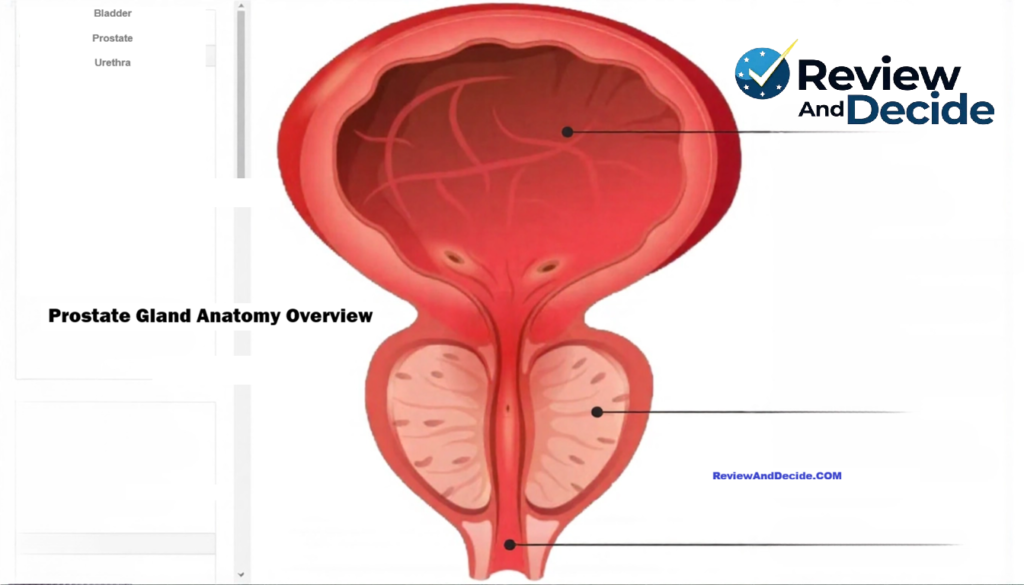
Understanding the prostate begins not with disease, but with anatomy and physiology. Before discussing age-related changes or research developments, it is essential to understand:
- Where the prostate is located
- How it develops
- What it produces
- How hormones influence it
- Why it changes over time
This article provides an in-depth, research-based overview of the prostate gland using information supported by institutions such as NIH, Mayo Clinic, and Harvard Health Publishing. It is designed for educational purposes and does not provide diagnosis or medical advice.
Policy Declaration
This article follows an educational publishing approach designed to comply with widely recognized standards for responsible health communication. Our editorial process emphasizes:
-
Evidence-aware explanations
-
Transparent sourcing
-
Neutral tone without exaggerated claims
-
Alignment with Google Helpful Content guidelines
-
Respect for YMYL (Your Money or Your Life) information standards
The purpose of this content is to improve public understanding of health-related topics rather than to promote specific medical products, treatments, or outcomes.
Before exploring specific details about the prostate, it is helpful to understand where this gland is located in the body and how its structure supports its biological functions. The prostate is a relatively small organ, yet its anatomical position and hormonal sensitivity give it an important role in the male reproductive system and in certain urinary processes.
[wpsm_ads1]
The following sections explain the anatomical location of the prostate, how the gland is structured, and how it develops and functions throughout different stages of life.
1. Anatomical Location of the Prostate
The prostate is situated in the lower pelvis, directly below the bladder and in front of the rectum. It surrounds the upper portion of the urethra — the tube responsible for carrying urine from the bladder to the outside of the body.
This anatomical relationship explains why prostate size changes may influence urinary flow. Because the urethra passes through the center of the prostate gland, structural changes in prostate tissue may affect the diameter of the urethral channel.
Medical references commonly describe the prostate as:
• Roughly walnut-sized in younger men
• Composed of both glandular and muscular tissue
• Located between the bladder and the pelvic floor
Although the prostate is not a large organ, its position within the urinary and reproductive systems gives it significant physiological relevance. Its influence comes primarily from its location and hormonal responsiveness rather than its overall size.
2. Structure and Composition of the Prostate
The prostate consists of several types of biological tissue that work together to support its functions.
These include:
• Glandular tissue, responsible for producing prostatic fluid
• Smooth muscle fibers, which assist during ejaculation
• Connective tissue, providing structural support
Anatomically, the prostate is divided into several zones:
• Peripheral zone
• Central zone
• Transitional zone
Research cited by the National Library of Medicine (NLM) indicates that these zones have distinct cellular characteristics and may change differently over time.
The glandular component produces prostatic fluid, while the muscular portion contributes to the mechanical process of ejaculation. This combination of glandular and muscular structures explains why the prostate participates in both fluid production and reproductive mechanics.
3. Development of the Prostate Over the Lifespan
The prostate develops gradually throughout life and is influenced by hormonal regulation.
Fetal Development
The prostate begins forming during fetal development under the influence of androgens, particularly testosterone. These hormones guide the differentiation of male reproductive tissues.
Childhood
During childhood, the prostate remains small and relatively inactive because hormone levels are low.
Puberty
At puberty, increased testosterone production stimulates rapid growth of the prostate. A hormone called dihydrotestosterone (DHT) — derived from testosterone — plays a central role in this process.
Harvard Health Publishing explains that DHT binds to androgen receptors in prostate tissue and influences growth during adolescence.
Early Adulthood
Following puberty, prostate size typically stabilizes for many years.
Midlife and Aging
Beginning in midlife, gradual hormonal shifts may again influence prostate tissue. Research suggests that DHT remains biologically active within prostate cells even as circulating testosterone levels decline with age.
These hormonal interactions are complex and vary among individuals.
4. Primary Functions of the Prostate
The prostate performs several biological functions within the male reproductive system.
4.1 Production of Prostatic Fluid
The primary function of the prostate is to produce fluid that becomes part of semen.
According to descriptions of male reproductive anatomy published by the National Institutes of Health (NIH), prostatic fluid contains:
• Enzymes
• Zinc
• Prostate-specific proteins
• Nutrients
This fluid supports sperm by helping:
• Protect sperm cells
• Enhance sperm mobility
• Contribute to semen liquefaction
Without prostatic fluid, sperm transport efficiency may be reduced.
4.2 Role in Ejaculation
The prostate contains smooth muscle fibers that contract during ejaculation. These contractions help propel semen into the urethra as part of the reproductive process.
4.3 Contribution to Fertility
While sperm cells are produced in the testes, their functional environment is influenced by fluids produced by accessory glands such as the prostate and seminal vesicles.
Prostatic fluid contributes to the biochemical environment that supports sperm viability.
4.4 Indirect Influence on Urinary Flow
Although the prostate does not produce urine, it surrounds the urethra. Because of this anatomical relationship, changes in prostate structure may influence urinary dynamics.
Because the urethra passes through the prostate, structural changes in the gland may influence urinary dynamics, sometimes contributing to symptoms such as frequent urination in men over 40.
5. Hormonal Regulation of the Prostate
Hormones play an important role in regulating prostate growth and maintenance.
Hormonal factors such as dihydrotestosterone (DHT) are often discussed in research exploring prostate tissue changes. Some individuals also review products covered in our prostate support supplement review while learning more about hormonal influences on prostate health.
Testosterone
Testosterone supports the development and maintenance of male reproductive tissues.
Dihydrotestosterone (DHT)
DHT is produced when testosterone is converted by the enzyme 5-alpha-reductase. Research published by the National Institutes of Health indicates that DHT binds strongly to androgen receptors in prostate cells.
DHT plays an important role in:
• Pubertal prostate growth
• Tissue maintenance
• Age-related prostate enlargement
However, scientific research on long-term hormonal influence continues to evolve.
Aging and Hormonal Shifts
As men age:
• Testosterone levels gradually decline
• DHT activity may remain locally influential within prostate tissue
This hormonal pattern is often discussed in relation to age-related prostate enlargement.
6. Age-Related Changes in the Prostate
The National Institute on Aging (NIA) reports that prostate enlargement becomes increasingly common after the age of 50.
This condition is called benign prostatic hyperplasia (BPH).
The term benign means that the enlargement is non-cancerous.
Important considerations include:
• Not all prostate enlargement causes symptoms
• Not all urinary symptoms are caused by prostate enlargement
• Prostate growth can occur gradually as part of normal aging biology
Medical research often discusses what causes an enlarged prostate, a condition known as benign prostatic hyperplasia (BPH), which becomes more common as men age.
7. Common Misunderstandings About the Prostate
Several misconceptions about prostate health are common.
Myth 1: Prostate Enlargement Always Means Cancer
Medical sources such as Mayo Clinic emphasize that most prostate enlargement is benign and not related to cancer.
Myth 2: Only Older Men Should Learn About the Prostate
Understanding prostate health can benefit men at different stages of adulthood.
Myth 3: Urinary Changes Always Indicate Prostate Disease
Urinary patterns may be influenced by many factors, including:
• Hydration levels
• Certain medications
• Urinary infections
• Neurological conditions
Only professional medical evaluation can determine the underlying cause.
[wpsm_ads1]
8. Current Research Areas
Research institutions such as the National Institutes of Health and Harvard Medical School continue to investigate several areas related to prostate health.
These include:
• Hormonal regulation of prostate tissue
• Inflammatory pathways
• Genetic risk factors
• Metabolic health connections
Many scientific studies identify associations rather than guaranteed outcomes.
9. Lifestyle and Broader Health Context
Harvard Health Publishing notes that several lifestyle factors may influence overall hormonal balance and systemic health.
These include:
• Balanced nutrition
• Physical activity
• Healthy weight management
• Metabolic health
However, no single lifestyle factor guarantees a specific prostate outcome.
Some individuals also explore nutritional compounds discussed in a detailed prostate ingredient analysis while learning more about prostate health research.
10. Prostate and Systemic Health
The prostate does not function independently of the rest of the body.
Its health may be influenced by broader physiological systems, including:
• Cardiovascular health
• Hormonal regulation
• Immune responses
• Inflammatory processes
Systemic health patterns may affect multiple organs, including the prostate.
11. When Professional Evaluation Is Appropriate
Persistent symptoms such as:
• Difficulty urinating
• Pain during urination
• Blood in the urine
should be evaluated by a qualified healthcare professional.
Only medical professionals can perform diagnostic testing and determine appropriate medical evaluation.
This article provides general educational information and does not replace professional medical advice.
Transparency & Scientific Context
Understanding the prostate gland and its role in male health requires consideration of multiple biological and medical factors. Scientific literature describes the prostate as a small reproductive gland that contributes fluid to semen and supports normal sperm function. Because the urethra passes through the prostate, changes in the gland may also influence urinary flow and related symptoms.
Medical knowledge about the prostate has developed through decades of clinical observation, laboratory research, and epidemiological studies conducted by major health institutions such as the National Institutes of Health (NIH), the National Institute on Aging (NIA), and academic medical centers worldwide. These studies provide insight into how prostate anatomy, hormonal regulation, and age-related tissue changes interact over time.
Research consistently shows that prostate growth may occur gradually as men age, often influenced by hormonal factors such as dihydrotestosterone (DHT). However, scientific evidence also emphasizes that the relationship between prostate size, symptoms, and overall health outcomes can vary widely among individuals.
For this reason, educational discussions of prostate health focus on explaining biological mechanisms and general research findings rather than predicting individual medical outcomes. Health conditions affecting the prostate can have multiple contributing factors, and proper diagnosis requires evaluation by qualified healthcare professionals.
This article presents information in a transparent, research-informed manner intended to improve understanding of prostate anatomy and function while recognizing the complexity of human health and the evolving nature of medical science.
What Science Consistently Emphasizes
Across major medical institutions and peer-reviewed research, several key points are consistently highlighted regarding prostate health:
-
The prostate is a gland involved in reproductive function and semen production.
-
It surrounds the upper portion of the urethra, which connects it to urinary flow.
-
Hormonal factors, especially dihydrotestosterone (DHT), influence prostate growth.
-
Age-related enlargement of the prostate is common and often non-cancerous.
-
Symptoms associated with prostate changes may vary widely between individuals.
Scientific literature also emphasizes that prostate conditions should always be evaluated by qualified healthcare professionals rather than self-diagnosed through online information.
Where Supplements Fit (Contextual Clarification)
Various dietary supplements and plant-derived compounds are frequently discussed in relation to prostate wellness. Some nutrients and botanical extracts have been explored in observational studies and clinical trials for their potential role in supporting general prostate health.
However, research findings are not always consistent, and supplements should not be interpreted as medical treatments or guaranteed solutions for prostate conditions. The effectiveness and safety of any supplement may vary depending on individual health status, dosage, and overall lifestyle factors.
Educational discussions of nutrients or supplements in this article are presented strictly in the context of scientific research and public health awareness.
Research Methodology
The educational material presented here was developed through a structured review of widely recognized health information sources and medical literature summaries. These sources include:
-
Government health institutions
-
Academic medical centers
-
Peer-reviewed research summaries
-
Clinical guidance from established medical organizations
The goal of this approach is to ensure that the explanations provided reflect widely accepted medical knowledge rather than anecdotal claims or promotional content.
No experimental medical recommendations are made within this article.
Editorial Transparency Statement
This article is published as part of an educational health content initiative focused on explaining biological processes, lifestyle factors, and research insights related to common health topics.
Content is created for informational purposes and is not intended to replace medical consultation, diagnosis, or treatment from qualified healthcare professionals.
Editorial decisions are guided by evidence awareness, neutrality, and responsible communication of health-related information.
Evidence Integrity Commitment
We are committed to maintaining a high level of informational integrity in all educational health content. This includes:
-
Avoiding exaggerated health claims
-
Avoiding fabricated clinical evidence
-
Avoiding guaranteed results or outcomes
-
Avoiding misleading interpretations of scientific studies
When scientific evidence is limited or evolving, language such as “research suggests” or “studies indicate” is used to reflect the current level of understanding.
Final Educational Summary
The prostate is an important gland within the male reproductive system that contributes fluid to semen and plays a supporting role in reproductive physiology. Because the urethra passes through the prostate, changes in the gland may also influence urinary function.
Research shows that the prostate commonly undergoes structural and hormonal changes as men age, particularly after the age of 40. These changes may or may not produce noticeable symptoms, and their impact can vary significantly between individuals.
Understanding the biological role of the prostate helps place age-related health discussions in context. Educational information can support awareness, but medical evaluation remains essential for accurate diagnosis and appropriate care.
Educational Intent Disclaimer
This article is intended for educational and informational purposes only. It summarizes publicly available knowledge related to prostate anatomy, function, and age-related changes.
The information provided should not be interpreted as medical advice, diagnosis, or treatment guidance. Individuals experiencing health concerns should consult a licensed healthcare professional for personalized medical evaluation.
Frequently Asked Questions (FAQ)
What is the prostate and what does it do?
The prostate is a small gland in the male reproductive system. Its main function is to produce fluid that becomes part of semen. This fluid contains enzymes, proteins, and nutrients that help protect sperm and support sperm mobility during reproduction.
Where is the prostate located in the body?
The prostate is located in the lower pelvis, directly below the bladder and in front of the rectum. It surrounds the upper portion of the urethra, the tube that carries urine from the bladder to the outside of the body.
Does the prostate change with age?
Research indicates that the prostate may gradually change in size as men age. Hormonal factors, including dihydrotestosterone (DHT), are believed to influence these changes, which commonly occur after midlife.
Is prostate enlargement always a sign of cancer?
No. According to medical sources such as Mayo Clinic, most prostate enlargement cases are non-cancerous. A common condition known as benign prostatic hyperplasia (BPH) can occur as part of the aging process.
Can prostate changes affect urination?
Yes. Because the urethra passes through the prostate, structural changes in the gland may influence urinary flow. Some individuals may notice urinary symptoms, although the presence and severity of symptoms vary.
When should someone consult a healthcare professional about prostate concerns?
A healthcare professional should be consulted if symptoms such as difficulty urinating, persistent urinary discomfort, or blood in the urine occur. Proper medical evaluation is necessary to determine the underlying cause.
Conclusion
he prostate is a small but biologically significant gland within the male reproductive system. It produces fluid essential for semen composition, responds to hormonal signals throughout life, and undergoes natural changes with aging.
Research from the National Institutes of Health, Mayo Clinic, and Harvard Health Publishing continues to expand understanding of prostate biology. While age-related changes are common, education and awareness provide clarity without unnecessary alarm.
Understanding what the prostate is and what it does empowers informed discussions with healthcare providers and supports a balanced, research-based perspective on men’s health.
[wpsm_ads1]
For additional research-informed articles covering prostate anatomy, hormones, and urinary health topics, visit our prostate health education hub.
Disclaimer
The content presented in this article is not intended to diagnose, treat, cure, or prevent any disease. Health information provided here is general in nature and may not apply to every individual.
Medical conditions related to the prostate or urinary system should be evaluated by qualified healthcare professionals. Always seek professional medical guidance regarding personal health decisions.
Medical & Educational Disclaimer
This article is provided for informational and educational purposes only. It is not intended to diagnose, treat, cure, or prevent any medical condition. The information presented is based on publicly available research and reputable health sources. Individuals experiencing health concerns should consult a qualified healthcare professional for personalized medical advice.
